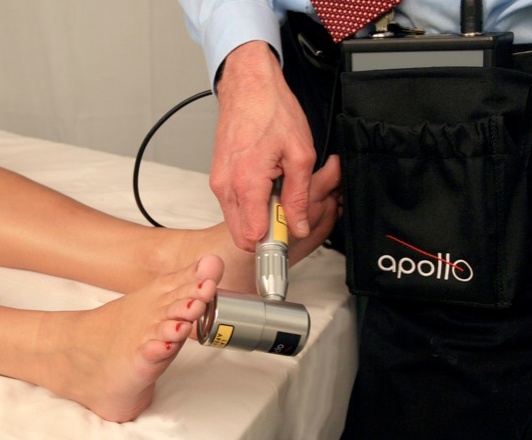
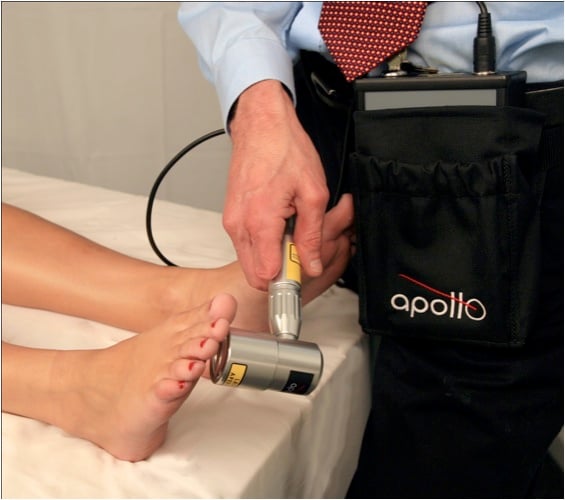
There’s no question that low-level laser therapy can help boost your practice by providing an added dimension that no other modality can do. And there’s also no question that you can bill for laser therapy—but there are issues that can make the billing process difficult.
 The primary concern is that laser therapy doesn’t yet have an assigned billing code that’s accepted by the insurance industry. However, it’s important to remember that many modalities did not have assigned codes—and didn’t for many years—until insurance companies decided to accept them (HIV or Lyme disease treatment are two that come immediately to mind).
The primary concern is that laser therapy doesn’t yet have an assigned billing code that’s accepted by the insurance industry. However, it’s important to remember that many modalities did not have assigned codes—and didn’t for many years—until insurance companies decided to accept them (HIV or Lyme disease treatment are two that come immediately to mind).
When to Bill
Billing is just one way to ensure low-level laser therapy is a profit center for your practice (more on that later). If you’re interested in exploring billing, make sure to first examine your case locally and statewide. Are you in a state where Medicare easily reimburses, or is there excellent workers compensation insurance or personal injury insurance in your area? Nationally, it is getting more difficult to be reimbursed, but if your particular region or state offers favorable insurance rates, it can be very profitable to bill.
When billing, the key point is to resist temptation to bill in a gray area as fines or even jail time are a possibility for improper billing. The following are the most common codes used by practitioners of laser and LED therapy. We are not recommending any particular codes and cannot advise you on billing issues.
- 97039: Attended Modality, Unspecified : This is a code that is also being used to bill for attended modalities. Reimbursement is good because it is understood to take more time than an unattended code. The problem with the code is that, being unspecified, it is occasionally rejected by some insurance carriers or hand audited. Make sure you have a one-page description of the treatment if a carrier wants more information. This is also the code that is often used for wound care. When the claim form goes out it will usually say something like: 97039: Attended infrared therapy or 97039: Attended laser therapy 97039-52 (less than 15 mins)
- 97026: Infrared: The beauty of this code is that it is for infrared light therapy. The problem with this code is that it is a code for a heat lamp and is a supervised, not constant attendance modality. Thus, reimbursement can be quite low, although for some practitioners, Medicare reimburses it. To improve reimbursement, try listing it as an attended modality or adding a –22 or an “unusual procedural services.” Two ways these codes can be used: 97026: Attended infrared light therapy 97026-22: Attended infrared therapy
- 97139: Unlisted Therapeutic Procedure : This code is for a therapeutic procedure meaning that the doctor must have one-on-one contact with the patient. The strength of the code is that it tells the insurance carrier that the doctor is spending direct treatment time with the patient. The weakness of the code is that an unlisted procedure is more likely to be closely inspected by an insurance carrier. Billing might look like: 97139: Infrared Stimulation: Constant attendance
- 97112: Neuromuscular Reeducation: This code is used for neuromuscular training to improve postural stability and control for functional issues, including reeducation of movement, balance coordination, kinesthetic sense, posture and proprioception. If laser is being used to foster this type of training and involves movement reeducation, it can be an effective code. This code is used correctly when the relationship of the procedure to sitting, moving or standing activities is evident. Many carriers have placed restrictions on the use of 97112 to patients with significant neurologic deficits. However, if there are neuromuscular problems and you use light therapy it is legitimate to use this code.
- 97140: Manual Therapy Techniques : This code is for a manual therapy technique meaning that the practitioner must have one-on-one contact with the patient and perform manual therapy. In this case the practitioner must be using light therapy as an adjunct to some type of manual therapy, including manual lymph drainage or soft tissue techniques. Because of the rounded head of the Apollo, you are performing massage while you are also performing a laser treatment.
If You Choose Not to Bill
The challenge with billing is that sometimes you will only be reimbursed for a portion of what you bill—while you are paying for full-time or contracting for part-time competent billing staff.
In response many practitioners are now choosing to offer low-level laser therapy on a cash-only basis. This can be another very effective way of bringing profit to your practice, even if your rates are low.
Because many patients do find that laser is helpful, yet are not able or willing to come in and pay the full fee, another option is to offer low-level laser therapy for rent at your practice. You can purchase a relatively inexpensive laser ($1,000 to $3000) and rent it to patients at a flat fee, say $50/week. You will likely find that demand is high—so much so that most patients are unwilling to give the tool back at the end of the week!—and in a short period of time, you can recoup your costs and establish another profit center.
Low-level laser therapy is fast becoming a widely accepted modality as patients recognize and demand its benefits. No matter how you charge, it’s clear that laser therapy is an essential part of today’s successful practice. 
Topics

Curtis is an internationally known expert in the field of laser therapy and author of "Light and Laser Therapy: Clinical Procedures," the authoratative text on clinical laser treatment. He has used lasers for 27 years, is the author of four books and more than 20 journal articles, and has lectured at many chiropractic colleges and state associations. He also studied various types of soft-tissue therapy with Janet Travell, MD; David Simons, MD; and Karel Lewit, MD.